The Genomics Research Programme
Initially we began our genomics research by sequencing just a small part of the DNA at Epilepsy Society, focusing on the exome, or 10 million letters that carry the most significant coding regions of DNA - those that direct the body to make proteins essential for it to function. This has helped us to make progress in recognising epilepsy syndromes, defining them genetically and understanding the correlation between patients’ genotype and phenotype. Now we are looking at the whole genome (3 billion letters comprising of coding and non-coding regions of DNA) in order to enhance our understanding of the genetic predispositions that cause different types of epilepsies. This could also help to identify risk factors and therapeutic markers, which could potentially lead to the development of new anti-epileptic medications.
Exploring genetic diagnosis for complex epilepsies
subtitle: Genomics
In this project we will undertake whole genome sequencing analysis of people with complex epilepsy. Our aim is to be able to give individuals participating in the programme an accurate diagnosis and provide the basis for developing individualised treatments.
Predicting and reducing the risks of avoidable deaths from epilepsy
subtitle: Genomics
Almost 1 in 100 people in the UK have epilepsy and they are 2-3 times more at risk of premature death and 20 times more at risk of sudden unexpected death compared to the general population. Our SUDEP project is undertaking whole genome sequencing on 100 DNA samples to try to identify genetic changes that may increase a person's susceptibility to SUDEP.
A multidimensional approach to epilepsy genomics
Alongside sequencing, we are using some of the most sophisticated equipment to help interpret genetic data. 3D stereophotogrammetry is helping to demonstrate how a genetic contribution to epilepsy can have a subtle but significant impact on facial structure and in turn help us to understand an individual’s genome; optical coherence tomography can show the impact of epilepsy on the thickness of the retinal fibres at the back of the eyes; and transcranial magnetic stimulation is helping to analyse brain activity without the need for electrodes or needles.
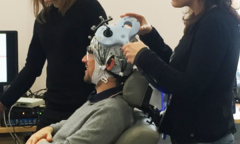
Transcranial Magnetic Stimulation (TMS)
subtitle: Genomics
Transcranial Magnetic Stimulation (TMS) is a non-invasive and painless technique, using a powerful magnetic field, similar to that used in an MRI scanner. This is used to stimulate a small region of the brain. For example, if we stimulate the brain region controlling movement, it will cause a measurable muscle twitch.
Our research
Neuroimaging
Neuroimaging enables us to look deep inside the brain to learn more about the impact of seizures on its structure and function.
Neuropathology
The Epilepsy Society Brain and Tissue Bank is the first of its kind in the UK. It is dedicated to the study of epilepsy through brain and other tissue samples.
Genomics
Read how we are working to understand the genetic architecture of each individual person's epilepsy through our world leading genomics research programme.